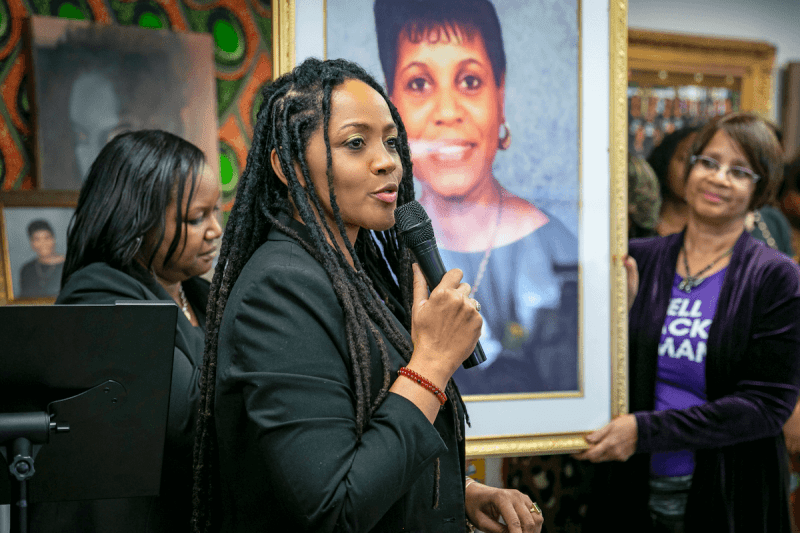Decades of ignoring this reality proves deadly for Black patients
Editor’s Note: This story is the second in a three-part series that looks at the disparities faced by African Americans who live in Wisconsin. In most cases, the disparities here are among the worst in the country. Since the killing of George Floyd, rallies that began solely to address systemic racism in policing are now broadening to call for reform in other areas.
Click HERE for Part 1 on disparities in the criminal justice system.
Click HERE for Part 3 on education disparities.
Earlier this month, Dr. Jasmine Zapata and her 9-year-old daughter, Aameira, marched with hundreds of others in Madison to draw attention to Wisconsin’s ranking as the worst state in the nation for Black infant mortality.
As the group made their way from the Capitol to SSMHealth Hospital on June 6, they passed the very entrance where she was brought by ambulance after going into preterm labor when she was a medical student.
“We were chanting ‘Black Mothers Matter, Black Babies Matter,’ and it was just so healing for me,’’ said Zapata, a UW Health newborn nursery hospitalist practicing at Meriter Hospital, where the march also stopped. “And it was so bittersweet to have my own preemie marching with me for maternal child equity.”
Aameria Zapata was born at 25 weeks, weighing a little more than a pound. She endured surgeries, a brain hemorrhage and infections before getting out of the hospital. Today, her mother says her “little miracle” is now “a brilliant girl, full of life,’’ who recently wrote a book.
But the story doesn’t end happily for far too many Black Wisconsin babies.
“I had to explain to her that her life matters, but that other Black babies who are born prematurely die at much higher rates, and some of them never get to come home from the hospital,’’ Zapata said.
While the overall infant mortality rate in the United States is lower than it was a decade ago, that decrease does not hold true for Black women in Wisconsin, according to a 2018 Centers for Disease Control and Prevention study that tracked data from 2013-2015 nationally.
That CDC study found Wisconsin has the highest infant mortality rate for Black women in the country. The infant mortality rate in Wisconsin, 14.28 infant deaths per 1,000 live births, is 1.7 times higher than the corresponding rate in the state with the lowest overall mortality rate.
Since the killing of George Floyd May 25 at the hands of Minneapolis police officers, protests that began in that city to decry police brutality have spread worldwide. The daily rallies continue, with African American organizers calling for system-wide changes in policing.
That call is extending to healthcare in Wisconsin. For too long, the nation’s healthcare system has collectively ignored the voices of African American patients, misdiagnosed or refused to believe their claims of pain, and used their bodies for research without their knowledge or permission.
“We Black women are sick and tired of being at the mercy of the U.S. healthcare system,” said Lilada Gee, founder of Lilada’s Living Room Saturday before a sea of white medical coats at a ‘White Coats for Black Lives’ rally at the Capitol. “When we have a medical need we are not heard and we are not believed. We are being undiagnosed, underdiagnosed and we and our babies are dying because of it.”
Infant Mortality Disparities
Despite the fact Dane County is one of the wealthiest counties in the state, data from Public Health Madison Dane County shows Black babies are still two times more likely than white babies to die before their first birthday.
“It is not acceptable to us that Wisconsin leads the nation in the Black infant mortality rate,” said Lisa Peyton-Caire, the founder and chief executive officer of The Foundation for Black Women’s Wellness that in January opened the Black Women’s Wellness Center in Madison. “I think folks are willing to step into that space now, like they never were before.”
One major reason for Black infants being born with lower birth rates and dying at a higher rate than white babies is the chronic stress Black women experience throughout their lives. In the medical profession, this correlation between chronic stress and its toll on the body is known as the allostatic load.
“I explain allostatic load as the systemic racism and the ultimate experience of chronic stress over the lifecourse,” Peyton-Caire said. “This constant stress gets down to a cellular level … it’s a constant withering away. Your body can no longer heal itself.”

A 2012 study by the National Institute of Health Institute drew a direct link between the allostatic load created by systemic racism and the health outcomes of African Americans.
Most telling was the discovery that health outcomes do not improve with wealth or other socioeconomic indicators or health behaviors.
This means a Black woman with a college degree earning $150,000 a year will still have similar health outcomes as a Black women with a high school diploma earning minimum wage due to the chronic stress of living in a racist society.
“Black women can eat vegetables, they can stop eating fried foods, they can walk five miles a day, jog, stop smoking, but we will still have babies born with low birth weights,” Peyton-Caire said. “The health outcomes will not improve because we are facing systemic problems.”
In March 2018, the Dane County Health Council initiated a community engagement campaign around the African American low birthweight crisis. The Council contracted with The Foundation for Black Women’s Wellness and its project partner EQT By Design to interview 300 African American women, men and youth in Dane County. The result, the Saving Our Babies report, was submitted to the Dane County Health Council in February of 2019.
The study found that the top two factors driving low birthweight babies and maternal and child health disparities were racism, discrimination and institutional bias followed by bias and cultural disconnect in healthcare delivery experiences.
“We need to invest in Black women. We need to provide security in the lives of Black women so we can live,” Peyton-Caire said. “When Black women are healthy, they become health advocates for themselves, they become health advocates for their families and they become health advocates for their communities.”
One of every three Black children in Wisconsin lives in poverty, a rate 3.5 times higher than the figure for White children. That difference is the fourth-largest in the U.S, according to the “Race in the Heartland: Wisconsin’s Extreme Racial Disparity, October 2019 report published by the Center on Wisconsin Strategy.
The report also found 85 percent of whites between 25 and 54 years of age are employed compared to 61 percent of Blacks in that age group. That disparity is the highest in the U.S.
Those who are employed face the third-highest income gap in the country, with the median white household income just below $60,000 while the median income for a Black household in Wisconsin is $29,000.
COVID-19 Exposes it All
The state’s chief medical officer and epidemiologist stood on the steps of the Capitol Saturday at the White Coats for Black Lives rally to ask his colleagues in the medical profession to join him in the recognition that racism is a public health crisis.
Dr. Ryan Westergaard said viruses move fastest through communities that have the fewest resources or tools to protect against them. That is proving true with COVID-19, he said, which has taken the lives of 169 Black Wisconsin residents. In all, 691 people in the state have died due to the virus.

“That means that being Black in Wisconsin increases your risk of dying from COVID 19 by 450 percent,” Westergaard told the crowd. “So what can we do about this, those of us who wear white coats? The first thing we can do is say it out loud: Systemic racism is a public health crisis. Systemic racism is causing people to die of COVID-19.”
As Westergaard points out, nothing so quickly lays bare the health disparities between white and Black residents of the state than the public health crisis associated with COVID-19.
“The way we think about it is that COVID-19 is another layer on top of long-standing inequities in conditions,’’ said Dr. Sheri Johnson, the director of UW-Madison’s Population Health Institute. “Segregation of housing prevents children from getting a quality education. The lack of healthy affordable food, poor living conditions. Those are the foundation for what we were seeing today in the burden of COVID-19 on those communities.”
African Americans also tend to be “essential front line workers,’’ holding jobs such as certified nursing assistants, bus drivers, EMTs, grocery workers, Johnson said.
“They are more likely to be in those jobs that are essential in a pandemic, but don’t have the protections that others enjoy,’’ she said “They don’t have necessary protections such as paid sick leave, support for child care. And those in high contact professions lacked masks and gloves. So their infection risk is higher and the protection measures aren’t in place.”

While underlying chronic medical conditions have been cited as reasons African Americans fare more poorly when exposed to COVID-19, Johnson points out that those underlying conditions occur at higher rates in the Black community because of long-standing inequities, poor housing and lack of opportunities to access healthy affordable food and safely exercise.
“Conditions like asthma, diabetes and high blood pressure don’t occur out of nowhere,’’ she said. “They occur because of the socio-economic conditions people live in. If you live in a house with mold, you’re more likely to have asthma.”
The PHI has What Works for Health web pages devoted to the best ways to improve community health, based on evidence. Economic changes such as paid family and sick leave and flexible scheduling top the lists.
“There are historic and ongoing structures that create advantage for some and disadvantage for others,’’ said Johnson, who held leadership roles in Milwaukee before moving to UW. “Let’s start with 300 to 400 years of being enslaved. Historical injustices have accumulated and result in the health outcomes you see now.”
Making Change Happen
Dr. Zapata is doing her part to keep the focus on the issue of healthcare disparities. She is the advisor to the group of University of Wisconsin School of Medicine and Public Health students who invited health care workers from across the state to participate in a “White Coats for Black Lives” rally Saturday at the Capitol.
“Even before George Floyd was murdered, racial inequities in maternal child health have been a long term struggle and problem,’’ she said.

Hospitals need a long-term commitment to dealing with racism, within the healthcare system and without, she said. It starts by changing the way people talk about racism and by acknowledging that everyone has implicit bias, she said.
“Racism is more than just the interpersonal,’’ Zapata said. “It’s bigger than that. We’re all part of a system that has racism embedded in it. Even just recognizing that is a start.”
Part of Zapata’s academic research involves interviewing Black women before, during and after pregnancy about their experiences in the health care system. The women are helping create a new model of maternal infant care, led by Black women, for Black women.
Through a grant from the Wisconsin Partnership Program, she has teamed up with Harambee Village Doulas and the African American Breastfeeding Alliance to start the “Today Not Tomorrow” pregnancy and infant support program.
The group began meeting at the East Side Community Center with informal gatherings of pregnant women, new mothers and women considering pregnancy. They enjoy music and share a meal with African American health care providers. They also share stories of their experiences in the healthcare system.
“It allows a place for Black women to heal from micro-aggressions they suffer in the healthcare system and to be part of a community,’’ Zapata said. “They need a safe space to heal and talk about these experiences.”
Since COVID-19, these gatherings have moved online. But the work continues, and Zapata says the goal is to enlist the patients as “co-creators” of a community-based movement to create maternal and child health care that is what the patients need and want.
One model is the Centering Pregnancy support group model, which has failed to catch on in the African American Community.
“We’re trying to get to the root of how we can shape the experience to meet the needs of Black women,’’ Zapata said.
Peyton-Caire agrees.
“I really want Wisconsin to become the model of health equity,” she said. “I want women who come to the Center to feel empowered, and I want Wisconsin to become the model for what a state can accomplish when it confronts the truth.”