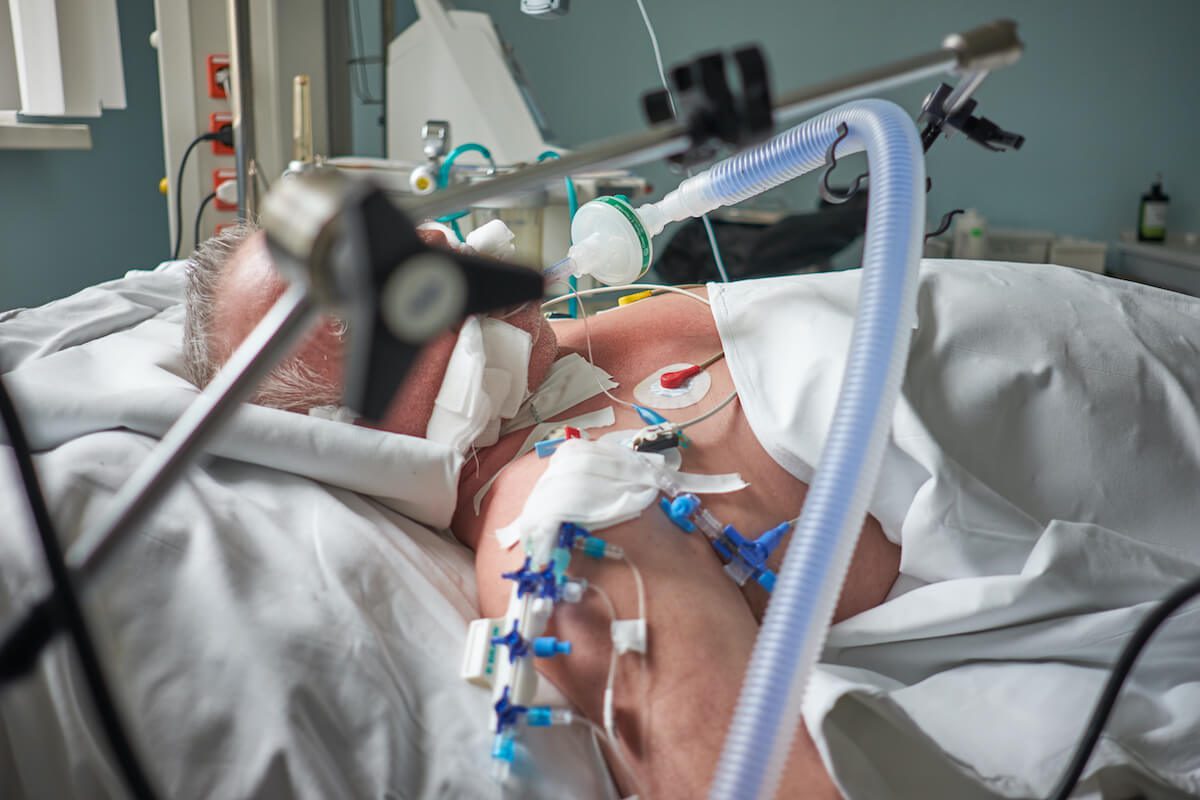
Hospitals across Wisconsin and the Midwest have few or no ICU beds available, putting patients at risk as numbers climb.
When Western Wisconsin Health has critically ill patients, officials at the hospital in the St. Croix County community of Baldwin try to transfer them to larger regional hospitals with intensive care beds and staffing to better treat them, external care sometimes necessary to save patients’ lives.
But finding available intensive care unit (ICU) beds at other west-central Wisconsin hospitals, or those in the metro Twin Cities across the border in Minnesota, has become akin to winning the lottery in recent weeks, hospital officials said.
A continued surge of COVID-19 cases, combined with existing health issues requiring hospitalization, has left hospitals in St. Croix County and many others across the state with few or no open beds. That means transfers of patients seriously sick with the coronavirus and other maladies to hospitals that can provide higher-level care often aren’t happening, placing those patients’ health—and, in some cases, their lives—at risk, officials at Wisconsin hospitals and other health officials told UpNorthNews.
“High-level intensive care units are currently overwhelmed with COVID-19 patients,” Western Wisconsin Health (WWH) CEO Alison Page said. “The inability to get really sick people to the level of care they need is causing bad things to happen and people to die.”
Early this year as it seemed the pandemic was receding, Wisconsin’s average number of daily COVID-19 deaths hit zero. With the current surge, the average daily death toll has jumped to 18—and it will likely get higher as hospitals continue to fill up, as deaths surge after hospitalizations.
One of those deaths nearly occurred last week at WWH, Page said. A woman patient for whom the hospital had been unable to find an ICU bed suddenly stopped breathing. WWH medical staff was able to save the woman, Page said, but other similar instances are likely as her hospital and others house more patients who need ICU-level care.
RELATED: Opinion: Healthcare Workers Are Dealing With Burnout and Trauma, We Need To Do More to Help Them
WWH has two ventilators and uses them only in emergency situations, Page said. Currently, one patient is on a ventilator, and the other vent may be needed soon, she said.
“That emergency situation is here now,” Page said. “We have a patient on a ventilator in Baldwin because there are no ICU beds available, anywhere.”
As evidence, on Sunday, Page said, she called 25 hospitals in Wisconsin, Minnesota, and North Dakota seeking an ICU bed for a middle-age man seriously ill with COVID-19. Not one of those hospitals had a bed available for her patient, Page said. He remains at WWH.
ICU beds in Wisconsin have been lacking for the past couple months and have become even more scarce in recent weeks as the virus continues to surge. As of Thursday, there were no ICU beds available in Wisconsin’s northwestern, western, and Fox Valley regions, and just one bed was free in north-central Wisconsin. Statewide, just 53 of 1,331 ICU beds were free.
As patients with COVID-19 and other illnesses requiring hospitalization continue to outnumber available beds, prompting overcrowding, Page and other hospital officials said they expect the situation could worsen, especially with the recent discovery of the Omicron variant. WWH and hospitals in St. Croix Falls and New Richmond are all beyond capacity and patients requiring hospital beds are instead kept in the emergency room.
With the number of new COVID-19 cases surging in St. Croix County in recent weeks, county Health Officer Kelli Engen has grown more worried as hospitals have become overwhelmed. Hospitalization numbers in the county—which recently had the third-highest virus infection rate of Wisconsin’s 72 counties—haven’t been this high since a virus spike last fall and early winter.
“The [COVID-19] infection numbers have been high for a long time now,” she said “and I’m concerned they’re not going to drop any time soon.”
‘Overwhelmed Right Now’
Other hospitals across the state report challenges finding available ICU beds as well. With nearly all of the larger regional hospitals that have ICUs full themselves, patients in need of critical care increasingly can’t access it in a timely manner, they said.
One Green Bay hospital turned away 28 patients seeking transfer there for ICU-level care on a recent day, a sign of overcrowding occurring at many Wisconsin hospitals, said Dr. Ashok Rai, president of Prevea Health Care. About 20% of beds at Prevea hospitals currently are occupied by COVID-19 patients, and combining them with an already high caseload that tends to peak at this time of year is creating a patient overflow, he said.
“Health care is not designed for having an extra 20%,” he said. “Our healthcare systems are overwhelmed right now.”
Eau Claire hospitals typically receive some of the patients from St. Croix County hospitals and others in the region seeking to transfer patients needing ICU care. But Mayo Clinic Health System-Eau Claire, Marshfield Medical Center-Eau Claire, and HSHS Sacred Heart Hospital have been at or above capacity for weeks, and their ICU beds are nearly always full and fill quickly when there is a vacancy.
Mayo Clinic hospital sites in the northwest region are always busy, and the increased patient load because of the COVID-19 surge has further strained existing resources, said Dr. Richard Helmers, regional vice president of Mayo Clinic Health System in Northwest Wisconsin.
At times, Helmers said, those hospitals can’t accept patients seeking to be transferred to those sites because of a lack of bed space, and they are sent to other hospitals. Mayo staff “take all steps possible to avoid these time periods,” he said, but they are at times unavoidable because demand for beds is outpacing availability.
Dr. William Melms, chief medical officer at Marshfield Clinic Health System, said system hospitals are at times turning away patients because of a lack of ICU and other beds. As demand grows, Marshfield is beginning to put two ICU patients in one room to accommodate more of them, he said, noting patient numbers have grown 20% during the past two weeks.
“We are a regional hub for referrals, and it’s very painful to have to turn people away,” Melms said. “We are doing everything we can, but it’s not enough.”
‘Fighting the Fight’
A lack of bed space isn’t the only challenge hospitals face as they attempt to care for more patients. Hospital officials said they have fewer staff members to care for patients compared to the surge a year ago, and patients infected with the Delta variant—who make up virtually all current cases—tend to be more sick and require more care than those hospitalized last year.
“Staffing is definitely an issue right now,” Rai said. “COVID patients are extremely labor-intensive.”
In addition, because nursing homes and other long-term care sites are full and have staffing shortages, transfers to those locations are being delayed, officials said.
Because they are more sick, patients hospitalized due to the Delta variant tend to need longer hospital stays, creating additional demand for hospital beds and staffing, Wisconsin Department of Health Services Secretary-designee Karen Timberlake said during a press conference Thursday. As a sign of illness severity, on Tuesday 688 patients statewide required ventilators, topping the previous one-day record of 638 set in November 2020, she said.
Melms said staffing is the biggest concern Marshfield hospitals face during the current surge. A nationwide nursing shortage and increased patient care needs has hospitals paying staff from other locations to try to meet demand. In addition, hospitals are shifting staff duties to provide more direct patient care, he said.
“Staff has been under tremendous pressure really since last November with the surge,” Melms said, “and, frankly, they are fried. We’re asking them to do more and more.”
Page acknowledged frustrations among healthcare workers asked to work more and longer shifts as high patient caseloads continue. Many of them are upset because most COVID-19 cases are preventable: Vaccinated individuals are 11 times less likely to be hospitalized and 15 times less likely to die than unvaccinated people, state data shows.
“In health care, we don’t pass judgement on our patients. We don’t judge; we care,” she said. “But I can tell you, healthcare workers everywhere are biting their tongues as they pick up extra shifts, exhausted, to provide care to people who are choosing not to be vaccinated … My message to these people is, ‘Put down your politics and roll up your sleeves.’”
Remaining optimistic amid the ongoing surge can prove challenging, Melms said. He said he finds a ray of hope in the fact that virus numbers fell off last spring more quickly than health experts anticipated, and he hopes that happens again. Additional vaccinations, including those now available to children ages 5-11, offer an additional reason for optimism, he said, noting “vaccination is really our way out of this.”
Rai acknowledged staff burnout at Prevea hospitals too, calling challenges healthcare workers have faced during the pandemic “a long battle.” With the Omicron variant posing additional likely challenges, it’s tough to predict when the surge will end.
“We’re doing everything we can to care for patients amid challenges,” he said. “We will keep fighting the fight.”