#image_title
#image_title
It is essential that patients, communities, and health systems advocate for policy solutions that will grow the health care workforce and expand innovative telehealth and home-based care programs, says local family doctor.
All of us understand that the COVID-19 pandemic has impacted every single Wisconsinite, whether through personal illness, the loss of a loved one, or the frequent disruptions in child care, school, and jobs.
What seems less understood are the clear ways in which the pandemic increasingly has affected medical professionals. In short, it has been really, really rough.
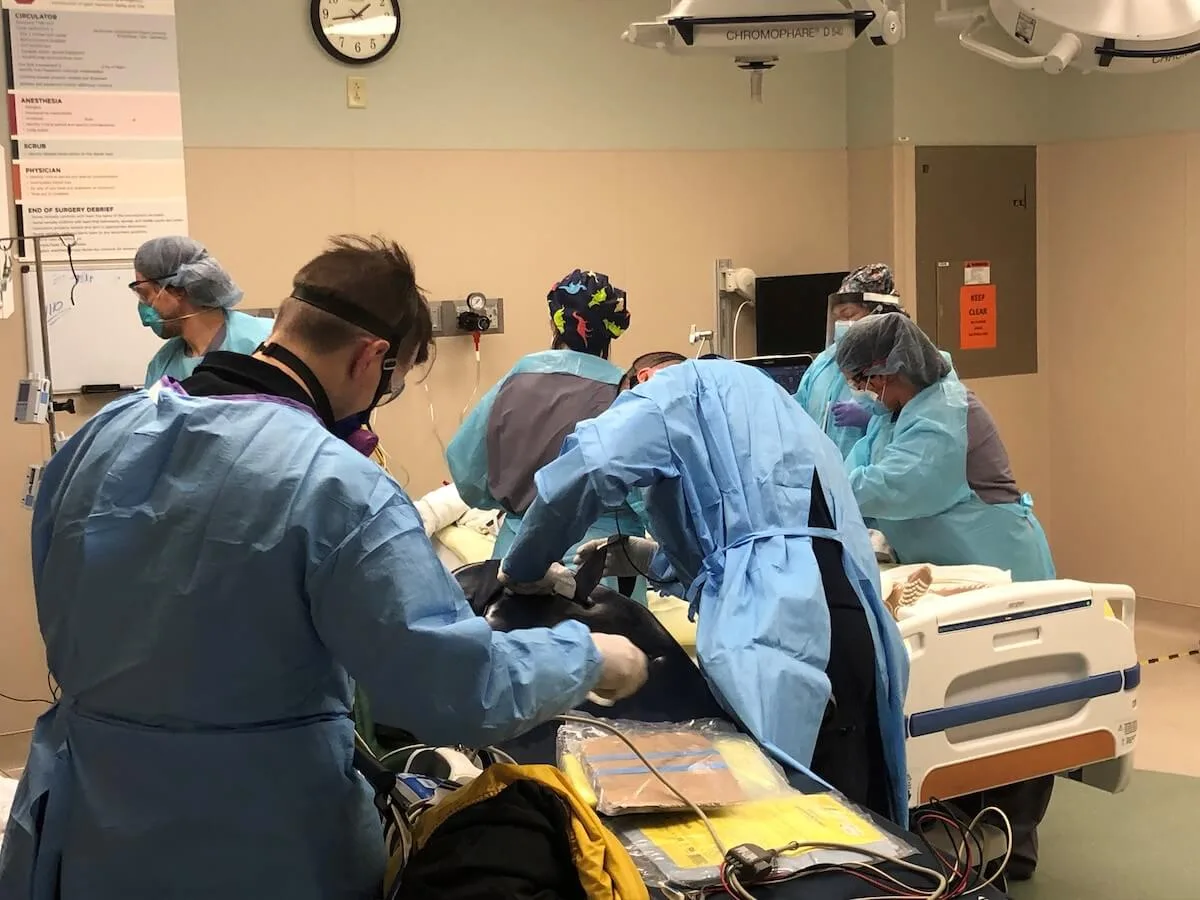
Healthcare workers who take care of hospitalized COVID-19 patients are dealing with burnout and trauma, but regardless of our clinical specialty or role in health care, most of us are “running on empty,” and the situation has become much more dire during this most recent Delta variant wave. We now know how to routinely transform our hospital units to take care of COVID patients, but the limiting factor for our capacity to care for all is our workforce strain.
Devastatingly, the toll of these past 18 months is increasingly revealing itself through transfers, vacancies, early retirements, and people leaving the profession. This vicious cycle leaves those of us remaining with even higher work burdens, and patients increasingly frustrated by long waits and at risk from the complications of delayed care. Throughout the COVID crisis, it has been healthcare professionals who risked their lives to save the lives of others, worked to the point of exhaustion, and worried about bringing the virus home to our families, but now, too, many of us need help ourselves.
It is no wonder so many medical professionals are struggling with trauma and loss due to their experiences at work. The tragic death of Dr. Lorna Breen underscores the difficult and sometimes fatal consequences that can occur when our caregivers’ health struggles largely go unnoticed or unsupported. State licensing boards should immediately address the impact of their application questions about mental health, which Dr. Breen’s family cited as a reason she struggled to get help.
Burnout and mental health challenges are contributing to the health professional shortage across the country. As more Americans grow older, there will be fewer doctors and nurses to care for the aging population and the increasing health consequences from delayed care during the pandemic. If we don’t take immediate action to address the shortage of healthcare workers, the emerging crisis will worsen, and our health systems will be burdened by the pandemic and its effects even longer.
The pandemic didn’t cause a health professional supply shortage, but it has exacerbated it. In 2017, Wisconsin had a physician burnout rate of 53.5%%—an alarming figure and far worse than the national average. Furthermore, Wisconsin ranks 28th in the country when it comes to the number of health professional shortage areas, with 110. That leaves many Wisconsinites vulnerable when it comes to accessing the health care they need.
New research shows this shortage is likely to get worse. A recent report by the Association of American Medical Colleges projects that by 2034, there will be a shortage of as many as 124,000 physicians, including up to 48,000 primary care physicians. More must be done to ensure that we reverse this trend before a deficit of medical professionals puts lives at risk.
This challenge is not limited to physicians. Nurses and other professionals working in clinics and hospitals are also overworked and at tremendous risk of burnout due to COVID. According to the US Bureau of Labor Statistics, America will need another 1.1 million nurses by next year to keep pace with the growing demand for care.
COVID exposed many of the longstanding inequalities that persist throughout health care, including the large number of rural, lower-income, and historically underserved communities that suffer disproportionately both from COVID and almost every other disease.
Given the magnitude of this challenge, it is essential that patients, communities, and health systems advocate together for policy solutions that will grow the health workforce and expand innovative telehealth and home-based care programs.
Health professional training programs must be expanded, and a combination of federal and state dollars currently support these programs. Congress is considering the Resident Physician Shortage Reduction Act, which would bring an additional 3,000 new doctors per year into the workforce through the residency training programs that we complete in our specialty after medical school.
President Biden has proposed federal efforts to increase the number of health professionals, improve access to care, and reduce health disparities in rural areas and communities of color. These initiatives taken together would be immensely helpful for every Wisconsinite and every American. These dollars and new initiatives should be targeted to grow the workforce in the areas that will provide the greatest positive impact on population health: primary care, behavioral health, maternal care, and geriatrics. Medicine in the 21st century is a team sport, so in addition to physicians and nurses, these funds should be used to grow training for other team members such as physician assistants, nurse practitioners, pharmacists, and community health workers, and develop the diverse workforce we need to establish trust with people of all backgrounds.
While we won’t solve the demand problems plaguing our healthcare system overnight, Congress can take steps right now to address burnout among physicians and nurses alike, safeguard the health of our medical professionals and guarantee all Wisconsinites will have access to a doctor and other essential health professionals when they need care.
Politics

New Biden rule protects privacy of women seeking abortions
Under the new rules, state officials and law enforcement cannot obtain medical records related to lawful reproductive health care with the goal of...

Biden marks Earth Day by announcing $7 billion in solar grants
The Biden administration on Monday announced the recipients of its Solar For All Program, a $7 billion climate program that aims to lower energy...
Local News

Stop and smell these native Wisconsin flowers this Earth Day
Spring has sprung — and here in Wisconsin, the signs are everywhere! From warmer weather and longer days to birds returning to your backyard trees....

Your guide to the 2024 Blue Ox Music Festival in Eau Claire
Eau Claire and art go hand in hand. The city is home to a multitude of sculptures, murals, and music events — including several annual showcases,...