#image_title
Legislation would increase federal funding for the kind of in-home nursing and personal care workers now in short supply and desperately in need.
Kelly Fouts hasn’t had a good—or even a full—night’s sleep in months.
Neither has her husband, David.
From the outside, the Foutses may seem like your typical suburban Waukesha County family. They have a nice home on a rolling wooded lot in Wales and spend much of their days navigating the busy lives of their four children.
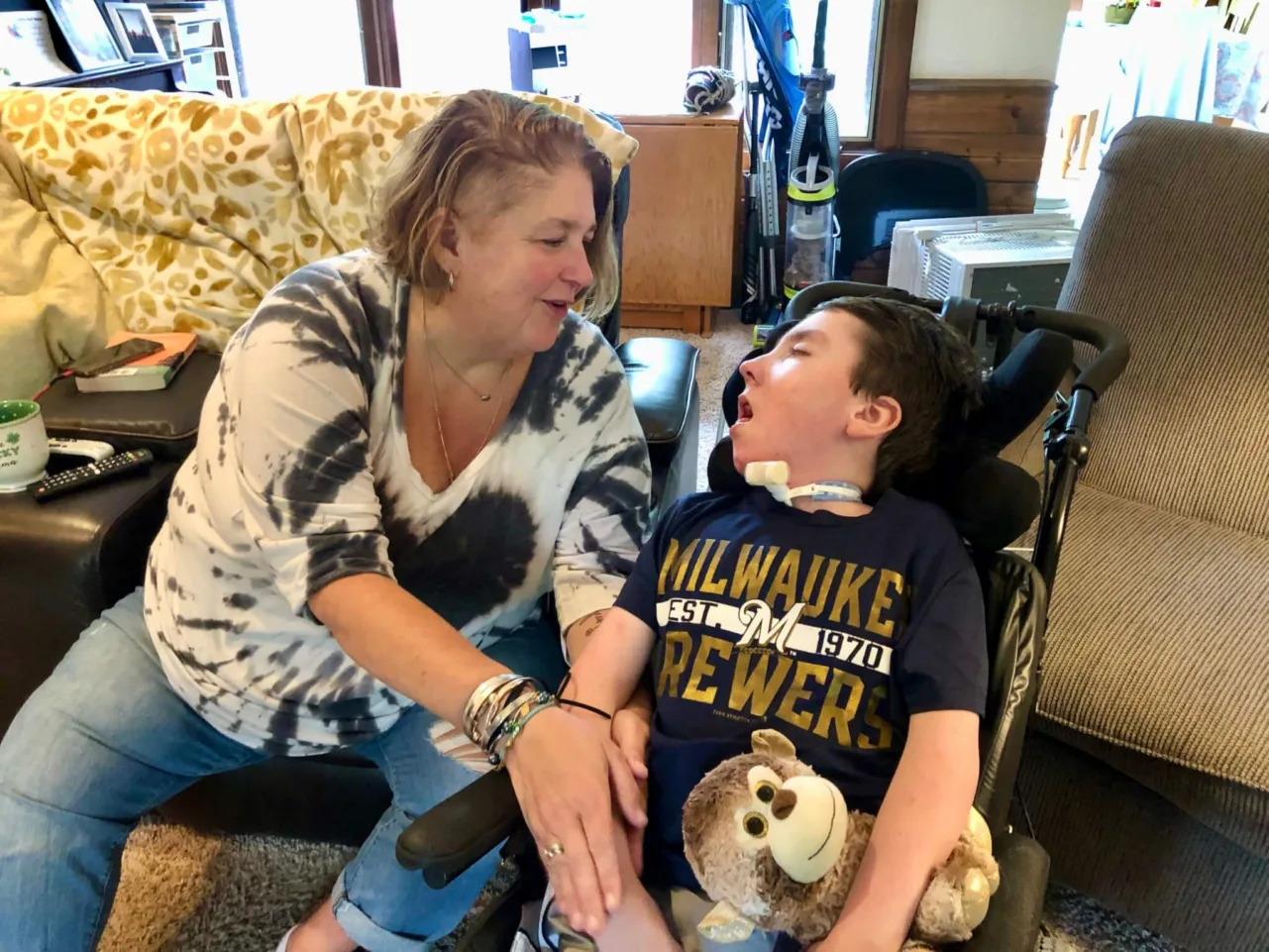
But what they need more than anything else these days is help caring for their 12-year-old son, Owen.
A victim of anoxic brain injury—the result of a non-fatal drowning he suffered at 16 months—Owen requires around-the-clock care. He cannot move. He has a gastrostomy-jejunostomy, or g-j, tube that provides food directly to his stomach, an ostomy for eliminating wastes, and tracheostomy tube that helps him breathe. He has rods in his back and suffers from a seizure disorder. Because of these complex needs, Owen requires skilled nursing care from a Registered Nurse (RN) or Licensed Professional Nurse (LPN).
Up until about five or six years ago, the Foutses had little trouble finding enough nurses to come to their home to cover most of the two 12-hour shifts needed to care for their son each day. Lately they’re lucky if they can find enough nurses to cover five of those 14, 12-hour nursing shifts. That means Kelly and David must provide the bulk of Owen’s care.
“It’s bad. It’s dire. The last time I posted on [Facebook seeking nursing help for Owen], I think the post was shared at least 1,000 times. We had two people reach out. Two people. And then one of them ghosted,” said Kelly. “I have a master’s degree in special ed. I haven’t worked in seven years [because I need to be here with Owen].”
The Foutses aren’t alone in their struggle.
Across the nation, hundreds of thousands of Americans are struggling to find in-home health and personal care workers.
Helping Hand
It’s the plight of families like the Foutses that’s made improving home-and-community based care for elderly and disabled Americans one of the goals of the Biden Administration’s Build Back Better legislation.
Currently being negotiated in Congress and scheduled for a vote as early as Friday or Saturday, the package would increase funding for a variety of programs aimed at improving the lives of families and individuals, including increasing the affordability of high-quality child care, making college more affordable for low-and-middle class students, and supporting families with their long-term care needs.
According to the White House, the measure would expand access to home- and community-based care to more of Wisconsin’s senior citizens and disabled citizens and improve the quality and wages of caregiving jobs.
That’s something plenty of Wisconsinites would like to see.

According to an August poll conducted by the progressive think tank Data For Progress, 67% of likely Wisconsin voters support the legislation, including 83% who would like to see funding go toward increasing access to long-term care for the elderly and disabled.
Most of those polled—between 68% and 76%—also support paying for the expanded benefits through some form of increased taxation on the super rich.
Attracting Workers
When asked what they would like to see from the plan, the Foutses said anything that could make private-duty nursing more attractive to RNs and LPNs would be a win. From where they sit, increasing the pay and incentives for private-duty nurses could go a long way towards doing just that.
Although states would be given a fair share of leeway in just how to use the increased Medicaid funding to provide more nursing and personal care to Americans, private-duty nursing is specifically mentioned as one of the areas they could put added Medicaid funding towards.
“It’s pretty thankless—doing private-duty nursing—truly,” Kelly said. “They get paid OK. But they have to pay their own taxes, because they get paid by the state [via Medicaid]. There is no paid time off. There is no vacation time. If our kid goes into the hospital, they don’t work and they don’t get paid. They also don’t get benefits.”
The family would also like to see funding to train more nurses, especially for in-home work, since they said many nurses do not even know private-duty nursing is an option when they get out of school.
RELATED: Paid Leave, Universal Child Care Help Employers and Employees Alike, WI Business Owners Say
Kathleen Papa, who sits on the board of directors for the Wisconsin Professional Home Care Providers or PHP—the state’s private-duty nursing association—and is the CEO of KPI, Inc., a home health care agency in Oconomowoc, agrees.
Increasing the pay of both skilled private-duty nurses, who make less than their hospital counterparts, and increasing the pay of CNAs and other personal care workers, who make on average less than $13 an hour in Wisconsin, would go a long way to attracting more workers to the fields, Papa said.
“We are all competing with hospitals that can provide huge incentives for relocation, or sign-up bonuses [to nurses] …The only way we can really even that playing field is to be able to offer more money,” she said.
A Real Need
Providing better pay could go a long way to reducing the backlog of families in the state awaiting care.
According to a Kaiser Family Foundation study, more than 3,100 Wisconsinites were on waiting lists for Medicaid-funded in-home health care in 2018. Nationwide, roughly 820,000 families in the country were on waiting lists for similar care.

The Foutses, who regularly post on private-duty nursing boards looking for nurses, have seen how the lack of in-home healthcare workers is impacting other families.
“There are probably thousands of people in Wisconsin right now looking for [in-home] nurses. And it’s adolescents and adults. I keep on seeing posts on private-duty nursing boards from the same man, I think he might be in the Fond du Lac area. He posts every other day that he needs help,” Kelly said. “He doesn’t want to go to a facility. He still works. But he has a vent, and he has a lot of other needs. Every time I read one of his posts, my heart just goes out to him, because I realize how fortunate my husband and I are, because we at least have each other to tag team this.”
But even with two people in the house to care for Owen, the workload is hard.
The stress often leaves Kelly posting on Facebook about Owen’s nursing needs in the off-chance others might share her pleas, or just venting in the middle of the night about what has become an untenable situation.
“This is a 24-hour-a-day job. It’s like running a hospital out of our house,” she said. “Somebody has to be able to help us. This life that we’re leading—and, like I said, we’re lucky because we have each other—is not sustainable. Staying awake for 48 hours, and then trying to do everything else that you need to do, is not a sustainable lifestyle for anyone.”

How CDC’s big changes to kids’ vaccine schedule could impact Wisconsin
The U.S. Centers for Disease Control and Prevention is dramaticaly reducing the number of vaccines it recommends to all American children, taking...

Congress gifts higher premiums to more than 300,000 Wisconsinites
By Judith Ruiz-Branch Heading into the holidays, hundreds of thousands of Wisconsinites will be burdened with wondering if they will be...

RFK Jr. ignores 100+ studies to push abortion pill ban—this is the mifepristone explainer you need
By Bonnie Fuller Apprehensive OB-GYNs across the country are alerting Americans that Health & Human Services Secretary Robert F. Kennedy Jr. may...

How to support Wisconsin residents as SNAP funding disappears
As the nation remains in a government shutdown, food assistance programs in Wisconsin are feeling the effects. FoodShare, Wisconsin’s federal...




