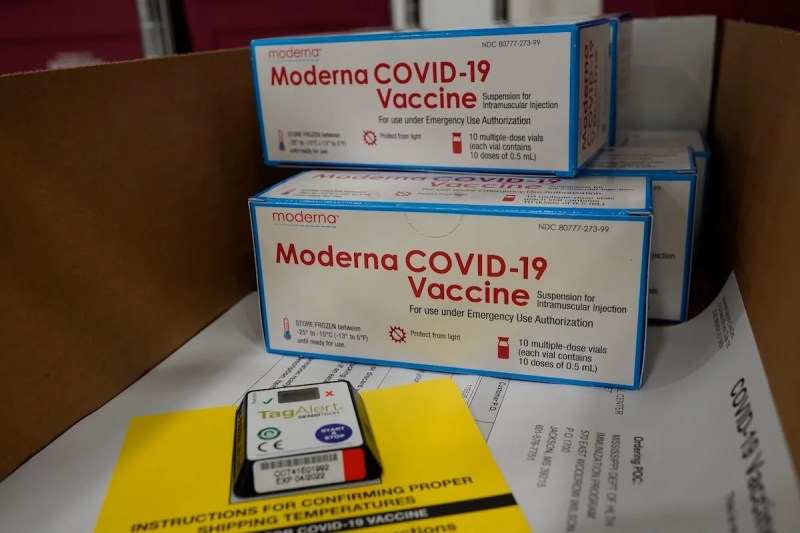
Slow pace that is driving divisive political rhetoric could change when President-elect Joe Biden takes office, launching $20 billion national vaccination program to vaccinate 100 million people in first 100 days.
While Wisconsin Republicans want to pin the slow rollout of the coronavirus vaccine in Wisconsin solely on the state Department of Health Services (DHS) and Gov. Tony Evers’ administration, the reality is more complicated, according to health industry professional who spoke at a recent committee hearing on the topic.
According to data from the Centers for Disease Control and Prevention, Wisconsin is behind other Midwestern states in distributing COVID-19 vaccinations. An article first reported by the Milwaukee Journal Sentinel based on CDC data further found Wisconsin ranked 10th out of 12 states in the Midwest in getting a first dose of the vaccine to its residents on a per capita basis.
Wisconsin also ranks 10th lowest in terms of how much vaccine has been distributed, per capita.
At 1,150 doses given per 100,000 residents in Wisconsin—or about 1.2% of the population—only Michigan and Kansas ranked lower for the rate at which its population was being vaccinated.
During his response to the governor’s State of the State speech on Tuesday, Assembly Speaker Robin Vos (R-Rochester) ripped into Evers’ management.
“Wisconsin doesn’t have a comprehensive rollout plan, few know where and when they can get a vaccine,” Vos said. “All of us deserve answers. With lives literally on the line, this is unacceptable.”
Since last week, distribution has sped up.
On Thursday, the Department of Health Services reported that out of the 607,650 doses allocated to Wisconsin, the state had received just over half, or 373,100 doses. Of that number, 195,152, or about 52%, have been administered, an increase from roughly one-third from last week.
Vaccination could continue to speed up when President-elect Joe Biden is sworn into office on Wednesday.
Biden announced Thursday evening that he wants 100 million vaccines administered during his first 100 days in office as part of a $1.9 trillion recovery plan that includes provisions to hire more public health workers for contact tracing and vaccine outreach.
“This will be one of the most challenging operational efforts we’ve ever undertaken as a nation,” Biden said. “We’ll have to move heaven and earth to get more people vaccinated, to create more places for them to get vaccinated, to mobilize more medical teams to get shots in peoples’ arms.”
Wait your turn
In a meeting Thursday of the Assembly Health Committee, Republican lawmakers asked DHS Assistant Deputy Secretary Lisa Olson about reports from their area pharmacists that they haven’t received doses yet. Later in the hearing, representatives from three pharmacy groups confirmed that they had not received doses of the vaccine.
The first vaccine to be distributed was the Pfizer vaccine, which requires ultra-cold storage to remain viable, so Olson pointed out that it could only be distributed to a limited number of facilities.
The second vaccine from Moderna, which can be refrigerated for up to 30 days after being thawed, has had about 200,000 doses set aside for the Pharmacy Partnership Program, a collaboration between the federal government and Walgreens and CVS to vaccinate long-term care facility residents and employees. States that enrolled in the program, including Wisconsin, had to agree to set aside half of the doses received until enough accumulated to implement vaccination.
Evers announced Friday that the first phase of the program, which focused on nursing homes, was launched in December and is expected to be completed by Monday. The second phase, which is focused on assisted living centers, was scheduled to begin Jan. 25 but the administration said pharmacies can begin once they have enough doses of the vaccine.
The remaining doses were sent to hospitals and healthcare facilities, so frontline healthcare workers could receive their shots, and to public health departments to distribute to independent healthcare workers.
Committee members repeatedly asked Olson about timelines and when the general public should expect to receive the vaccine. Olson announced that in February, DHS will launch a site where people can register for the vaccine, but as far as timing is concerned, that depends on the federal government. DHS does not control how many doses of the vaccine the state receives. DHS is notified week-by-week how many the state will receive, making long-term planning difficult.
“Today I could not tell how much vaccine we will receive the first week of February,” Olson said. “We cannot tell [vaccine administrators] how much they will be receiving until Friday because of the system at federal level.”
Federal officials have been reserving vaccines to ensure second doses. Biden’s transition team announced it was prioritizing first doses to get as many people vaccinated as possible.
Apples to oranges
Wisconsin is not the only state that has struggled with the rollout of the vaccine due to the way distribution is being handled at the federal level. Olson explained that it’s a numbers game, and the federal government is calculating the numbers.
While states are mostly distributing vaccines to a group designated “1A,” which includes frontline health care workers, long-term care workers, and long-term care residents, the number of doses a state receives is based on its total population size, not the size of the 1A group.
As an example, Olson noted Wisconsin has the same number of people in its 1A group—around 550,000—as West Virginia. But because Wisconsin’s overall population is smaller than West Virginia’s, the number of doses Wisconsin is receiving is smaller than West Virginia’s. As a result, it will take longer for Wisconsin to completely vaccinate group 1A.
Also, in terms of the overall number of doses allocated to Wisconsin per capita, Olson said the state is about the middle of the pack and is receiving fewer doses than other states of comparable size. South Dakota has one of the highest immunization rates in the country, but it also received more doses per capita than Wisconsin and many other states. New Jersey is also much further along than Wisconsin, but it has received 654,900 doses so far, of which it has administered 264,681.
John Raymond, president and CEO of the Medical College of Wisconsin, testified that the vaccination differences between states at this point are, “insignificant in terms of reaching herd immunity,” which he said could take a year to reach.
DHS has authorized over 1,200 facilities enrolled vaccinators across Wisconsin, Olson said, they just need more doses from the federal system.
“We are eager to receive more vaccines in Wisconsin,” Olson said. “The question mark for us is when. We have the system, we have the infrastructure in place. We are ready to go.”
In his State of the State response, Vos lamented that Wisconsin didn’t have an innovation said he’d heard about in Texas.
“I talked to my aunt and she said, ‘Have you gone on the website to find out what your place in line is so you know when you’ll get the vaccine?’” Vos recounted. “I literally said, ‘I don’t know what you’re talking about. We don’t have that in Wisconsin.’”
They don’t have that in Texas either, at least not at the state level.
Lara Anton, a spokesperson with the Texas Department of Health Services, said maybe one of the state’s 50-plus health departments has implemented something along those lines, but Texas’s DHS has nothing that matches Vos’s description.
“Texas is decentralized so I wouldn’t want to entirely rule out that this is happening in a smaller city or county that is coordinating vaccine rollout for their jurisdiction,” Anton said. “It’s not happening at the state level because we have distributed vaccine to a wide variety of providers across the state.”
Vos also pointed to Arizona, where the State Farm Stadium in the Phoenix area is being repurposed as a 24/7 vaccination hub. He did not mention the $1 million donation from the Ben and Catherine Ivy Foundation that helped it happen, along with support from the Arizona Cardinals, Blue Cross Blue Shield of Arizona, Arizona State University, and the Arizona Department of Emergency and Military Affairs.
Politicians Pitting Inmates Against Grandma
Another topic of discussion between legislators and health officials was the composition of vaccination priority groups, including the recommended 1B vaccine group proposed by the State Disaster Medical Advisory Committee’s (SDMAC) vaccine subcommittee.
Olson said this week her department has opened up the 1A group to include police and firefighters for health departments that have already completed 1A and have vaccine left.
SDMAC had made its recommendations for who should be included in the next round, 1B, of vaccinations people over the age of 70; IRIS and Family Care recipients, who commonly have intellectual or developmental disabilities; public-facing essential workers, such as non-EMS first responders, educators and child care providers; and people living in congregate settings such as prisons, employment based housing (typically for farm workers), transitional housing and shelters for either the homeless or people seeking refuge, such as domestic violence shelters
The inclusion of “incarceration facilities” has attracted politician rhetoric across the country and worldwide.
“The subcommittee met today,” Vos said, “and decided that prisoners should get the vaccine before your 65-year old grandmother.” The Speaker urged people to provide comments to DHS on the suggestion.
The Advisory Committee on Immunization Practices (ACIP), a federal agency providing guidance on vaccine distribution, recommends that individuals 75 and older be included in 1B; SDMAC expanded the group to those 70 years and older. The Trump administration has been pushing for vaccines to be opened to anyone 65 and older, though some health officials have argued that allowing people in their late 60s to be part of 1B could slow the rollout to other vulnerable groups.
SDMAC’s proposal explained that age is, “the single greatest risk factor for mortality due to COVID-19.” The agency cited evidence that, compared those those ages 18 to 29, those between the ages of 75 and 84 are eight times more likely to require hospitalization and are 220 times more likely to die from COVID-19; those who are 85 and older are 13 times more likely to need hospitalization and are 630 times more likely to die.
Individuals between 65 and 74 are five times more likely to require hospitalization and 90 times more likely to die.
“So their immunization is also recognized as a pressing priority limited by vaccine availability and the significantly large number of individuals in the group,” the Agency wrote.
Due to the size of that population, estimated to be about 176,006 in Wisconsin according to the Census, the agency decided to split the difference and expand 1B down to people age 70 and older based on DHS data.
By comparison, Wisconsin’s prisoner population is small; only about 20-24,000 individuals are held in custody at any given time at facilities that employ around 4-5,000 correctional officers. But the infection rates of those facilities are staggering; according to the Department of Corrections’ website tracking COVID-19 infections, 10,554 inmates, 25 of whom have died, and 2,339 correctional officers have tested positive for COVID-19 since the pandemic broke out.
Ed Wall, former cabinet secretary at the Department of Corrections under former Gov. Scott Walker, was not surprised by the infection rate, given how difficult it is for prisoners to social distance in their tight quarters.
“When you look at the prison system, with 24,000 people in the system you have a breeding problem there,” Wall said.
One advantage of vaccinating this population is that it’s also relatively easy to carry out, which is one reason the majority of the subcommittee agreed to add them to 1B. Wall also pointed out it would reduce the risk of spreading the virus to the outside community via corrections officers and their families.
Wall didn’t want to weigh in one way or another, but he’s not surprised that Vos framed the issue the way he did.
“I would expect it from a politician,” Wall said. “It’s always going to be a hard sell for anybody. It’s the same issue when you talk about air conditioning in prisons. Well, we have people in the general population without air conditioning, why are we giving air conditioning to prisoners?”
SDMAC is accepting public comment on the proposed 1B groups through 4 p.m. Monday. Public comments can be submitted to DHSSDMAC@dhs.wisconsin.gov and the committee asked that “vaccine subcommittee” and “Phase 1B” be included in the email subject line.