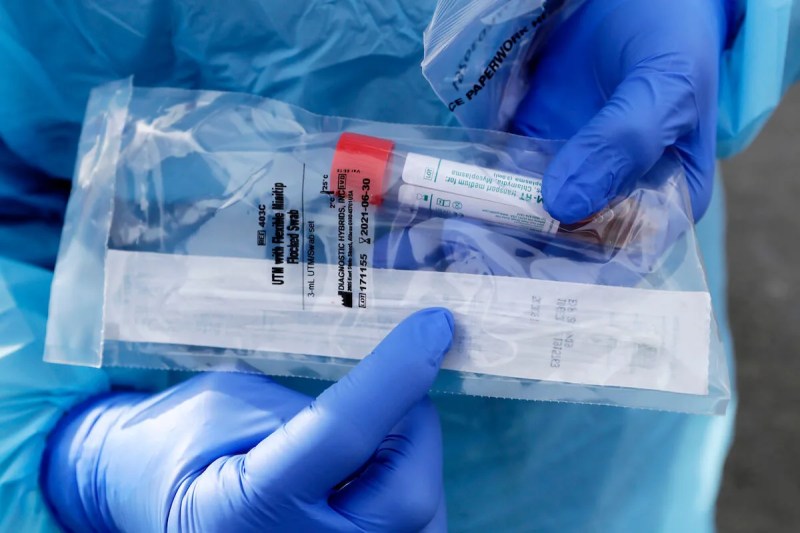
A Los Angeles man whose wife died of coronavirus is now in quarantine with symptoms. He still cannot get a test.
After celebrating their retirement with a month-long trip to Asia, Loretta and Roddy returned to the U.S., landing at Los Angeles International Airport on March 8. They planned to stay with Roddy’s sister in the greater Los Angeles area for two nights before returning to their Orlando, Florida, home on March 10.
Instead, Loretta fell ill on March 9. Roddy tried to revive her using mouth-to-mouth resuscitation and then called 911. Lorena was rushed to the Pomona Valley Hospital Medical Center, where she died of the coronavirus the next day. She was 68.
Now, over a week later, Roddy, who is 72, is in self-quarantine with symptoms of the virus but is still unable to get a test, the Los Angeles Times reports. The Los Angeles County department of Public Health said Loretta’s positive test result for the coronavirus, which led to her death, was not enough for Roddy to receive a test—even though he performed CPR on his wife.
“What’s really frustrating is the fact that this is a man who was as close as you can get to the virus and we’re struggling with trying to get him properly tested,” Rem, Roddy’s son, told the LA Times.
The family asked the LA Times not to use their last names “for fear of being shunned or targeted.”
Roddy’s story highlights the catastrophic failures of the Trump administration and the Centers for Disease Control and Prevention to provide widespread and readily available tests for COVID-19, the disease caused by the novel coronavirus. America’s first confirmed case of the coronavirus came on Jan. 21 in Washington State, but President Trump initially declined to pursue more aggressive testing for the disease out of fear that more positive cases would hurt his re-election effort.
The president also downplayed the severity of the virus for six weeks, comparing it to the flu. The CDC also botched the development of its first coronavirus test and is still struggling to develop enough tests. The Trump administration has since allowed private and academic labs to develop their own tests, which has increased the pace of testing, but the shortage remains massive and has allowed the disease to spread like wildfire.
Nearly two months into the coronavirus crisis, it’s still nearly impossible to get a test in the United States—unless of course you’re an NBA player, celebrity, influencer, or otherwise wealthy or powerful person.
A 34-year-old North Carolina woman told COURIER she asked her doctor in late February to test her for coronavirus after she developed flu-like symptoms, including a bad cough, but tested negative for strep and the flu. At the time, she was told she didn’t meet the criteria. Later, she learned that several people at a recent conference she’d attended in Boston were diagnosed with COVID-19.
“I think given that I tested negative for the other things, bringing me back in to be tested would have been the right thing,” said the woman, who asked to withhold her name. “I’m young and otherwise healthy. Didn’t have any shortness of breath. But what if I do have it and I’ve been spreading it for two weeks because someone didn’t want to test me even though I asked?”
“What if I do have it and I’ve been spreading it for two weeks because someone didn’t want to test me even though I asked?”
If anything is clear about the current state of the pandemic, it’s that Roddy and the North Carolina woman are not alone. There’s story after story after story of people being denied tests, even though they’re symptomatic or have had contact with infected individuals.
On March 7, President Trump said “Anyone who wants a test can get one.” That was untrue then and more than 10 days later, it remains untrue. The American testing shortage is so dire that a Chinese woman living in Massachusetts who fell ill with coronavirus was forced to fly to China to be tested after she was denied testing three times at her local hospital.
The shortage of tests isn’t the only issue. In some places in the U.S., there’s also a shortage of chemicals used to process the tests and limited lab capacity. And then there’s the miles of red tape people have to jump through.
In Los Angeles County, for example, the Department of Health mandates a person must fall into one of the below categories to be tested:
- Have a fever or symptoms of respiratory illness and have been in close contact with a confirmed case over the past 14 days
- Have a fever or symptoms of respiratory illness and are a healthcare worker without an alternative diagnosis
- Have symptoms requiring hospitalization and a history of travel from affected countries (China, Iran, Italy, Japan, and South Korea) in the last 14 days or other imaging tests indicating a viral pneumonia but no alternative diagnosis
- Be part of a cluster of acute respiratory illness within a group living environment, such as a nursing home or homeless shelter
If patients don’t fit the county’s criteria, a doctor can theoretically work with a private lab to have a test processed there, but even these commercial labs are running low on tests, and providers have said it is nearly impossible to get tests for patients. The bureaucratic hurdles that one must jump through in order to get checked are immense, as detailed by a New York Times writer who tested positive for the coronavirus.
And yet, people like Roddy, a non-insulin-dependent diabetic with a heart condition, who have had direct contact with infected individuals and are symptomatic still can’t get tested. Roddy’s running a low-grade fever, but his temperature isn’t high enough for it to be considered a symptom, his family told the LA Times. Instead, Roddy remains in quarantine at his sister’s house along with his sister and brother-in-law, both of whom are also symptomatic.
The family said that medical personnel at the hospital and nurses and epidemiologists from the Department of Public Health have been helpful and supportive, but haven’t been given enough resources.
“The people who need the tests aren’t getting them,” Cathrina, Rem’s wife, told the LA Times. “The big issue is whoever is managing however these tests are distributed … is not aligned with those who truly need the help.”
Editor’s Note: This story has been updated to include context for why Roddy and his family did not provide their last names to the Los Angeles Times.