#image_title
#image_title
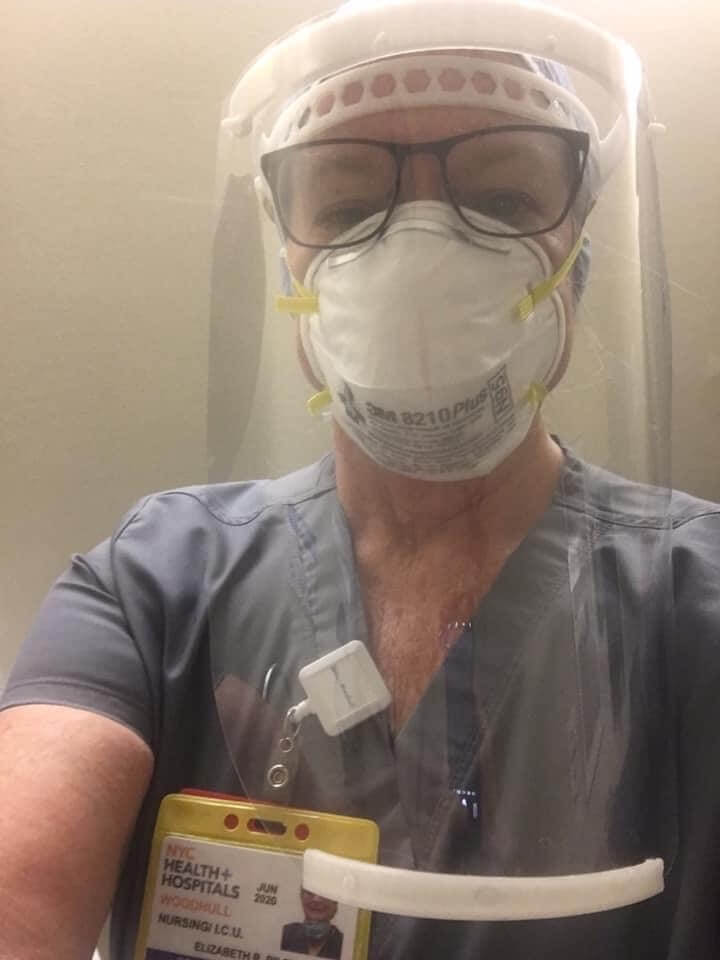
Buffy Riley experiences the harsh realities at the current center of the outbreak
Editor’s note: This is the third in an ongoing series of stories profiling Wisconsin resident Elizabeth “Buffy” Riley and her three weeks working as a nurse in New York. Read Part 1 and Part 2 of the series here.
“Buffy” Riley knew it was coming. She had seen news reports of bodies piling up at New York hospitals as the coronavirus pandemic stretched its deady grip ever further. She had heard about semi-truck trailers being parked outside hospitals, virtual mortuaries on wheels.
Since arriving in New York on April 2 in response to a nationwide call for nurses to help out at hospitals there overwhelmed by COVID-19, Riley had at first waited for a hospital assignment, then worked in an intensive care unit packed full of patients barely hanging on. She plans to help treat patients hospitalized with the virus for three weeks.
On Monday, her first day in that ICU unit at Woodhull Medical and Mental Health Center in New York, Riley was struck by the death-like pallor of the patients there. All of them required ventilators to breathe. All of them were hooked up to central lines, necessary to pump high-powered medications through their bodies to fight back against the deadly virus attacking their lungs. All of them looked like death warmed over.
But they didn’t die. Riley and her fellow nurses did anything and everything they could during their 12-hour shifts, scrambling to keep death at bay. At night they met to review the care they provided, seeking to help patients as much as possible, trying to keep them alive.
Then, on Wednesday, it happened. One man in the room where Riley was working died. About two minutes later, so did another.
“I knew as sick as these people were, there were going to be deaths,” Riley said late that night from her New York hotel room, where she tried to recover from the rigors of her day. “It was going to happen. But you’re never ready for them to die.”
Riley’s experience in a hectic New York hospital in the eye of the COVID-19 storm is a far cry from her work at Cumberland Memorial Hospital, located in a northwestern Wisconsin city of about 2,200. Her work there rarely involves ensuring the safety of people sent home from the hospital. Life-and-death situations are rare.
But in New York, where Riley is treating people stricken with serious coronavirus cases, the specter of death is ever present. On Thursday the number of COVID-19 cases in New York state increased by 10,000, to 159,937, more than in Spain or Italy, European nations hit hard by the virus.
More than 7,000 people in New York have died from the virus, and an estimated 20,000 have been hospitalized. Most of those cases, deaths and hospitalizations are in the city of New York.
In the U.S., 462,000 cases have been confirmed, with about 16,500 deaths.
Riley’s first day in the ICU unit at Woodhull nearly did her in. The room was a blur of beeping and blinking monitors, alerting nurses to a list of patient needs impossible to keep up with. The people Riley and other nurses there provide care for straddle a thin line between life and death as COVID-19 ravages their bodies.
“Oh my God, I don’t know how I’m going to do this for another 17 days straight,” Riley said Monday night, her body aching from a 12-hour shift trying to keep up with a seemingly never-ending effort to keep patients alive.
But Riley showed up for work the next day, boarding a bus at 5 a.m. that would bring her back to Woodhull. On Tuesday she consoled a woman patient who was sedated and needed a ventilator to continue breathing. Her husband had just died.
Unsure whether the woman could hear or sense her, Riley stood at her bedside, holding her hand, and spoke to her through her mask.
“We are taking care of you,” Riley told the woman in a soft voice. “You’re in good hands. God is watching over you.”
Then it was time to move on to another patient.
Later, Riley was told not to spend so much time with any one patient, a sign of the harsh realities of New York hospitals overwhelmed with intensely sick, contagious COVID-19 patients. Doing so increases her chances of catching the deadly virus, Riley was told, and potentially spreading it to others.
And there are always more critically ill patients to care for, a fact underscored by Riley’s final grim-yet-appreciative assessment of her day: “I didn’t kill anyone.”
‘Really, really sick’
By Wednesday Riley was feeling more familiar with her ICU space. She knew where to find various items of medical equipment. She knew the routine. She had developed a better rapport with her fellow nurses.
She also had, perhaps subconsciously, adapted her mindset to her new unforgiving environment. She had started to reassess what “really sick” meant.
“I am already getting somewhat immune to how sick these people are when I talk about them being stable, if that makes sense,” Riley said. “Like it’s no big deal. But it is a big deal. They are really, really sick.”
Part-way through her day Riley was switched to another unit, where the central line came out of one patient as the woman woke from sedation. Riley reacted quickly and fixed the situation, saving the patient from intense pain.
As the number of patients critically ill with COVID-19 were admitted to Woodhull Wednesday, they packed the already-full ICUs past capacity. Those who still required ventilators to breathe but were deemed less at risk of imminent death were transferred to another space, and Riley was sent to help monitor them.
“It’s a sign of how many really sick people there are here,” she said.
Later that day she was switched to yet another room, the one where two men died within minutes of each other.
When asked how those deaths impacted her, Riley said “So far it’s only two deaths … Ask me after I lose two more.”
On Thursday morning, shortly after Riley arrived at Woodhull, a patient stopped breathing. A short time later he was dead.
Later in the day a young man whom Riley described as “strong and vital” was admitted to her ICU. A chest X-ray showed his lungs were severely damaged by COVID-19, with only about 25 percent of his lung capacity remaining, his lungs choked with the thick, inflammatory material that hinders breathing.
“The X-ray of his lungs was absolutely horrifying,” she said, noting she won’t be surprised if he dies too.
‘The right thing’
Riley’s grim work in New York has its high moments. She credits her fellow nurses at Woodhull for their diligence, for their dedication to keeping patients alive, for risking their lives to save others. After long hard days, Riley appreciates the little things: a laugh with the nurses at her hotel, a few hours of sleep, her own coffee brewer to help energize her early mornings.
“We now have our own bus!” she texted excitedly Wednesday morning. “And we don’t have to be on it until 6 a.m.! I can sleep until 5:30, get my coffee now that I have a brewer, and meet the day in a lot better mood!”
The rigors of her demanding days are a struggle for Riley. After working all day with only a brief lunch break, she feels every bit of her 62 years. Her muscles and joints ache and cramp, the pain exacerbated by moving patients so heavily sedated on medications they can’t assist at all. On her bus ride back to her hotel room each evening, Riley sags heavily into her seat, her nursing work having taken its toll.
But this morning, Good Friday, she was back on the early morning bus again, fueled by another cup of coffee, headed back to Woodhull for another day of trying to stave off death.
She knows her day will be hard. She knows it will be filled with loud beeping machines, people yelling, far more stress than she is used to dealing with. She knows her body will ache. She knows her heart will too, as she works with people sicker than she ever imagined. She knows she is likely to encounter death.
But she goes anyway, just like she has every day since being assigned to Woodhull. She does it because it’s her way to help, she said. She does it because it’s the right thing to do.
“This is an extremely challenging experience,” Riley said. “But you just have to think about how you would want your mother or child to be treated, and then it is not so difficult. You just do the best you can.”
Politics

New Biden rule protects privacy of women seeking abortions
Under the new rules, state officials and law enforcement cannot obtain medical records related to lawful reproductive health care with the goal of...

Biden marks Earth Day by announcing $7 billion in solar grants
The Biden administration on Monday announced the recipients of its Solar For All Program, a $7 billion climate program that aims to lower energy...
Local News

Stop and smell these native Wisconsin flowers this Earth Day
Spring has sprung — and here in Wisconsin, the signs are everywhere! From warmer weather and longer days to birds returning to your backyard trees....

Your guide to the 2024 Blue Ox Music Festival in Eau Claire
Eau Claire and art go hand in hand. The city is home to a multitude of sculptures, murals, and music events — including several annual showcases,...